Physiotherapist and bestselling author and YouTuber Will Harlow shares some causes of back pain, including sciatica, and what you can do to find relief.
Words: Will Harlow. Images: Hay House and Shutterstock.
Through my work as a physiotherapist, I have become known as a specialist in helping people with back problems and sciatica. One of the reasons I have had more success than most practitioners when it comes to treating sciatica is that my approach is very different to those you might find online, or in your average clinic.
Once I’ve assessed my patient and decided that nothing “sinister” is causing their sciatica, I tell most people to disregard completely the typical stretches they’ve seen online. Why? Because these exercises are largely ineffective for most of the people I help – and may even make the problem worse!
If you look online, the typical approach towards exercises for sciatica begins by stretching the muscles in the affected leg.
The problem with this approach is that it often only serves to aggravate it. The reason for this, I believe, is the following: it has become clear to me over years of treating patients that nerves absolutely hate to be stretched. When you stretch a nerve, you aggravate the area, which can cause inflammation to increase. Unfortunately, most of the stretches recommended for sciatica don’t just stretch the muscles in the leg – they stretch the sciatic nerve too.
In the process of attempting to do something good (stretching the muscles), we inadvertently do something bad (stretch the nerve). This leads either to no change, or to symptoms getting worse. Either way, the result is not good for the person who diligently went searching for a way to fix their problem. (This is another reason why I tell my clients not to rely solely on YouTube videos for the most part, even my own!)

A different approach
Luckily, I’ve found a far more effective way of helping people with sciatica. It’s not perfect and it isn’t effective every time, but it works more than the usual approach.
It’s very simple. I focus my client’s attention on stretching the non- painful leg… while leaving the
painful leg well alone.
I know this is an unusual concept, but there’s some recent evidence to support my theory. The human body is very clever and we’re starting to see proof of the fact that when you make a change on the left side of your body, in some circumstances a similar change happens on the right side, too. We aren’t sure how this happens, but there may be some kind of mirroring effect going on, due to complexities in the human brain.
Another reason that could explain this is that when we’re in pain, certain parts of our body compensate for the areas that aren’t working well. This often means that our right side can become tight and restricted even when it’s our left leg that’s hurting. By stretching the right side, we can often indirectly help the left leg. This approach also means that we avoid aggravating the painful leg and everything calms down as a result.
It’s important to note that the following exercises aren’t suitable for everyone and there’s no way for me to tell if they’ll help you or not. It’s vital you get checked out by your doctor or physio before putting these exercises into action. Here are two of the common stretches I recommend to my clients with sciatica:

Glute stretch
For this long-sitting glute stretch, start sitting on the floor (either unsupported as shown, or with a wall at your back for comfort). Fold the leg to be stretched (the non-painful side) over the other leg and plant the foot on the floor. Grab the knee with your opposite hand and pull towards your opposite shoulder until you feel a stretch in your buttock (on the non-painful side). Hold for 30 seconds and repeat four
to five times.

Piriformis stretch
In this piriformis stretch, you are going to work your non-painful side (in this picture, that’s the right leg). Lie on your back with your knees bent. Now, cross the non-painful leg over the painful leg, so the non-painful shin is in contact with your opposite thigh. Reach through the gap between your legs and pull your painful leg gently up towards you as shown in the picture. This will lift the non-painful leg into a stretch that targets the gluteal muscles and the piriformis muscle. Hold for 30 seconds, repeating five times each day.
The downside of sitting
It’s no secret that working an office job where you sit in a chair for eight hours, five days a week, 48 weeks of the year, or where you just sit a lot at home, has the potential to place you at risk of having a bad back. But why is this the case? Surely people who keep their backs immobilised for most of the day avoid “wear and tear” or “sprains and strains” far better than more active workers?
Well, that is true to some extent. Being immobile is the only sure-fire way to avoid the kind of sprains and strains more active individuals risk suffering. However, don’t let that fool you into thinking sitting is risk-free. Every job has its own unique profile of health risks. Sitting has a different, more insidious effect on our backs.
Feeling stiff? Try these four stretches for your hips!
For a start, in the absence of bouts of exercise done regularly before or after work, sitting for long periods of time, day after day, causes you to lose a lot of the muscle strength in your back and midriff. This area is referred to collectively as your core.
The core acts as a sort of corset to keep your spine and midriff stable when you move. It’s a vital part of your anatomy. Sitting doesn’t involve much core stability, so if all we do is sit, the core gets weaker and weaker over time through disuse. This weakness can leave us vulnerable to back trouble as soon as we put any significant stress on the spine, such as when lifting something heavy.
The other reason that sitting can be bad for our backs comes down to our evolution as humans. We weren’t built to sit – we were built to walk, squat and run. When we sit, several of the muscle groups in the hip and pelvis are put into a shortened position. Over time, if nothing is done, this shortened position becomes permanent. This may contribute to the fact that, in one study, almost half of all office workers reported being uncomfortable with their work station at their job.
The muscles at the front of our hips, called the hip flexors, are significantly shortened when we sit. If we sit a lot, they remain tight even when we stand up. This can lead to a tilt in the pelvis, as the tight muscles pull the pelvis forwards. We call this an anterior pelvic tilt, which is a fancy term to describe the “duck-bottom” appearance that some people have when they walk around – characterised by bums and tummies sticking out.
This position can put stress on the back when held for a long period of time. It may be one of the most common factors contributing to back pain in office workers. The problem is, this postural change happens so slowly that no one notices. However, try looking at yourself side-on in a mirror: is your bottom sticking out? Are the bony points at the front of your hips tilted forwards? If you answered yes to either of these questions, you could be suffering with an excessive anterior pelvic tilt.
If you think you might be developing this issue, don’t panic! There are a few things you can do to combat the effects of sitting and to reverse gradually the postural change you have developed.
First, it’s important to try to minimise unnecessary sitting from this point onward. You might not be able to change your job, but you can minimise the length of time you spend sitting outside of work.
The other alternative is to get a standing desk for your workplace. These desks give you the option of standing up while you work. They represent a great way to break up the eight hours of sitting we may do during a working day.
If you are going to sit for long periods, it’s important to stretch the tight areas at the front of the hips to prevent this tightness from building up and tugging the pelvis or tilting it forwards. There are a couple of simple stretches you can do regularly to counter the effects of sitting. One of the best ones is the hip flexor stretch.
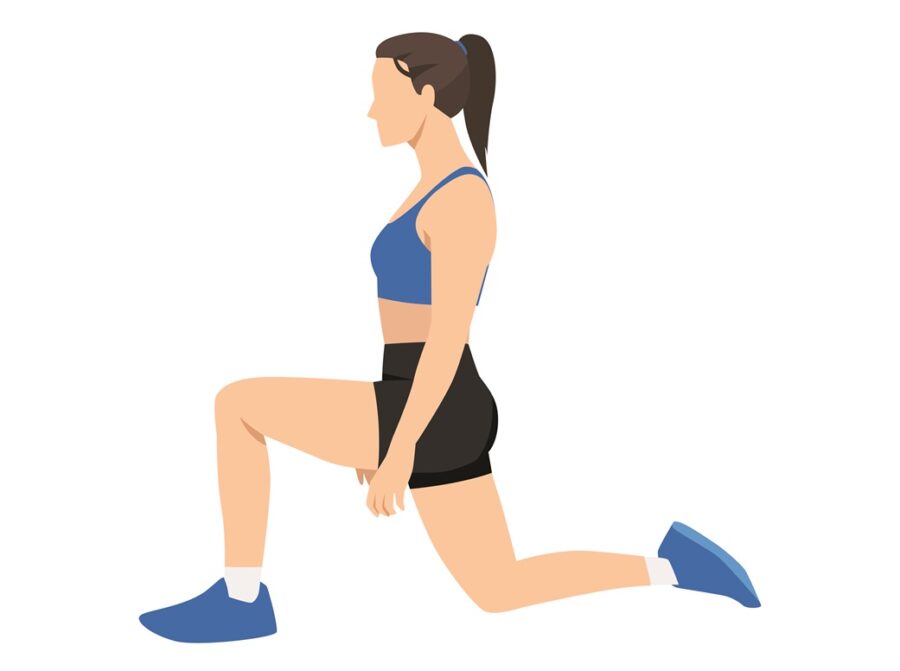
Hip flexor stretch
Begin by kneeling, with the knee of the leg to be stretched resting on a soft floor. Keeping a straight back and a tall kneeling posture, gently squeeze your buttocks and ‘roll’ your pelvis underneath you. You should feel a stretch at the front of the kneeling leg, near the hip. Hold this position for 30 seconds, repeating several times a day on each side.
Read more in Thriving Beyond Fifty: 111 Natural Strategies To Restore Your Mobility, Avoid Surgery And Stay Off Pain Pills For Good (£19.99, Hay House), out now. See Will in action at youtube.com/@HT-Physio.








